Stories
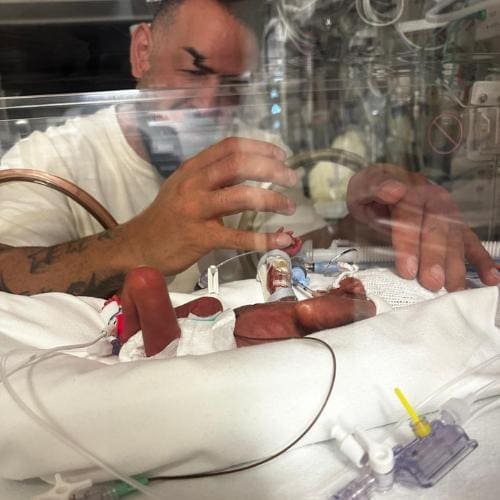
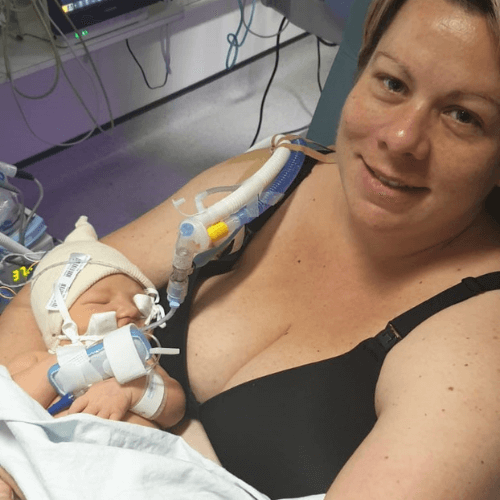
Take courage from our unique stories
Read the inspirational and moving stories about Ickle Pickles here.
Take courage or comfort from these unique stories and consider sharing the story of your Ickle Pickle for others to read.

Stay informed with Ickle Pickles
Whether you’re a parent, sibling, uncle, aunt, grandparent, or family friend, we invite you to share the story of your Ickle Pickle. Each NICU journey is unique, and we welcome contributions from anyone touched by premature birth or experienced in neonatal care.
Latest Ickle Pickles News
The good, the great, and the awesome
Explore Ickle Stories
Take 10 minutes and be inspired
Get in touch Today
Get involved & become a friend of the Ickle Pickles!