Austin’s story
At my 20-week scan, I was told that my baby Austin measured small so I was referred to Southampton Hospital for a specialist scan. It confirmed that although he was measuring small, he was okay and I would be scanned again at 24 weeks at my local hospital in Chichester.
At my 24-week scan, which was now in COVID lockdown, panic set in with the maternity team. I was immediately admitted to the labour ward. I was told that Austin would be born that day. Chichester Hospital could not care for babies so small so I was transferred to Portsmouth Hospital. My husband was allowed to accompany me and met our wonderful consultant Laura Fulwell-Smith who looked after us so well.
After rigorous scans and checks, our baby was diagnosed with severe IUGR: Intrauterine Growth Restriction. I was suffering from Pre-eclampsia which causes high blood pressure and Oligohydramnios (a disorder of amniotic fluid resulting in decreased amniotic fluid volume). We also had reverse or intermittent end-diastolic blood flow to the cord, meaning my placenta was working inefficiently and the blood flow to Austin was restricted, and getting worse. This meant Austin needed to come out very soon but luckily not on that day. He was healthy but just not growing much at all.
I had to be super aware of any changes in his movement. The neonatal team decided that he could stay in a little longer because each week would make such a big difference to his health once he was born.
I spent the next four weeks travelling to and from Queen Alexandra Hospital in Portsmouth. Every week I was checked, scanned and monitored between three to five times. Each time, I did not know if it was going to be the day he was born. My bag was always ready and packed in my car.
Gradually, the condition of my placenta was worsening and the blood flow was decreasing.
We had booked my C-section for 29 weeks and five days but we did not make it that far. At 28 weeks and three days, I had not felt Austin move much that day so I went to Portsmouth Hospital to be checked. He was doing okay but as his movement pattern had changed considerably, the consultant on duty decided it was too risky to leave him in any longer.
Austin’s premature birth during COVID
The next morning at 28 weeks and four days Austin was born weighing just 710 grams. Austin’s IUGR meant that he weighed much less than an average 28-weeker.
Because of COVID restrictions, there was a debate about whether or not my husband was allowed to be with me. He was only just allowed to be present in theatre.
I only knew that Austin had been born when I saw him being whisked out of the door to my right to the waiting neonatal medical team. We were told nothing until I heard him cry sometime later when I was being taken to the recovery area. That was all we knew of him for some time. We didn't even get to see his face.
We were only given a card with a photo of our baby. Until I was feeling well enough to visit the Neonatal Intensive Care Unit (NICU) much later that evening that was all we had or knew of our tiny son.
That was also the first and only visit my husband was allowed for over three weeks. He was allowed to meet his son just once! COVID rules meant only mothers were allowed to visit the NICU and even then for only 2 hours a day.
I was the only one allowed to see Austin which made me feel immensely guilty and distraught. My Husband only got to see his newborn tiny son through video calls and photos.
Eventually, the rules changed slightly and both parents were allowed to visit. But still only one parent at a time so we never got to be at his bedside together whilst Austin was being cared for at Queen Alexandra Hospital.
Austin’s NICU journey
Austin's journey, like many others, was full of ups and downs.
He suffered a suspected Necrotising enterocolitis (NEC) infection - a serious condition, where tissue in the bowel (small and large intestines) becomes inflamed - at two weeks old. Thankfully it was diagnosed and treated before it did any real damage.
Austin had suspected Cows Milk Protein Allergy (CMPA/dairy allergy) and needed numerous blood transfusions. He needed help to breathe constantly. He struggled to feed and put on weight consistently for most of his hospital stay.
He had more injections, cannulas and blood tests than most adults have in their lifetime.
It is unbelievable how quickly I got used to the noises in the Intensive Therapy Unit (ITU) and all the brain scans, ROP (Retinopathy of Prematurity) eye checks, blood gas checks, jaundice and picking up signs that baby is struggling or having a better day.
Between the bad days, I suddenly got a glimmer of hope. Austin was finally big enough to move back closer to home to Chichester Hospital. This was the first time his Dad and I could be with him together as a family, except our daughter. This was a huge lift and helped us to stay positive.
Preparing to come home
We spent almost four weeks at St Richard's Hospital in Chichester. We learnt how to adjust for life at home. Austin had to learn how to bottle feed. We had to learn about how to support Austin at home and signs to look out for as he would be coming home on Oxygen. We even had to learn how to bathe him - he was so small and sensitive as very premature babies often are.
Austin spent a total of 79 days in hospital and came home the day before his due date.
COVID changed everything for us during this time.
There were no NICU support groups, no parents chatting or leaning on each other for support or friendships built. At hospital, the parents' room was closed off and it was not possible to stay at hospital with your baby until discharge.
COVID ruined so many milestones and firsts. The first time Austin met us, his parents, we had masks on. But for all the negatives - and there were a lot - we are just truly thankful that Austin received the best care possible during an immensely challenging time for all the staff at both hospitals that helped him.
Austin is now a happy, healthy, albeit slightly small 3.5-year-old and most people comment that they wouldn't know he was so premature if I didn't tell them!








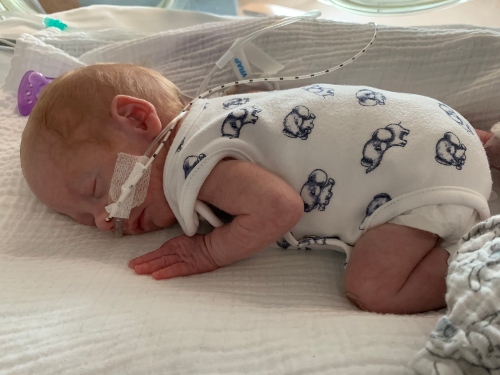
.jpg)









.webp)
.jpg)
